InterStim™
Made by Medtronic
www.medtronic.com
Sacral neuromodulation is a reversible therapy used to treat overactive bladder, urinary incontinence, and incomplete bladder emptying. As of 2018, the InterStim device is the only FDA approved sacral neuromodulation device in the US, but several others are in development. The InterStim device consists of a small battery that is implanted under the skin in your buttock, which sends mild electrical pulses via a wire that sits under the tailbone, near the sacral nerves. These nerves control the bladder and the muscles related to urinary function. The pulses sent by the InterStim device help smooth out overactive connections between the bladder to the brain, which can lead to an improvement in overactive bladder symptoms.
Indications
InterStim therapy is used for patients with urge incontinence, urgency, and frequency who have failed other treatment options. It is reserved for patients who have not had adequate improvement in behavioral therapy or medications. It is a third line option along with PTNS and BOTOX.
In addition, Interstim can be used for urinary retention and fecal incontinence. Patients who have both urinary and fecal incontinence are often encouraged to consider InterStim, as it may improve both problems. More information regarding this can be found on Medtronic’s website. Click here for a link.
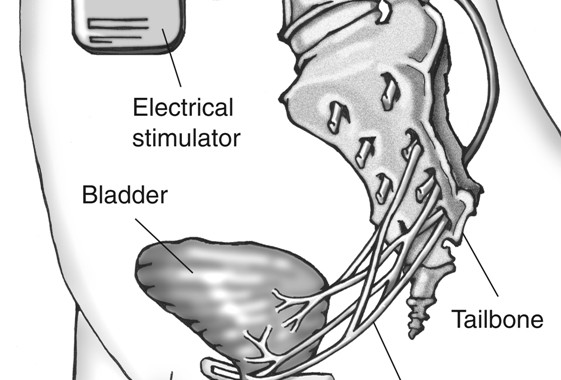
How it Works
A small battery (about the size of a pacemaker) is be placed under your skin. This delivers mild electrical pulses to the nerves that control your bladder. This therapy works by stimulating the sacral nerve (near the tailbone). This nerve carries signals between the brain and the bladder. In overactive bladder, these nerve impulses can occur too frequently. Sacral neuromodulation uses a “bladder pacemaker” to smooth out these overactive signals, which can improve OAB symptoms.
Procedure
Placement of the InterStim device is a 2 stage process. The first step is a minimally invasive test either done in the office or ambulatory center under local anesthesia in which involves placing one or more leads through the skin of your lower back to a location under your tailbone. These connect to an external battery pack that is either taped to your skin or worn on your clothing by clipping it to your waistband. You return to see your doctor four to fourteen days later to discuss how well it worked. You and your doctor can then determine if moving on to a permanent implant would be beneficial.
If the testing phase is successful, a permanent InterStim implant can be placed. This procedure involves finalizing the lead placement and implanting a small permanent battery under the skin.
Results
- 84.8% improvement in urgency urinary incontinence.
- 39% of patients need revision of the sacral neuromodulation implant
Al-zahrani AA1, Elzayat EA, Gajewski JB. Long-term outcome and surgical interventions after sacral neuromodulation implant for lower urinary tract symptoms: 14-year experience at 1 center. J Urol. 2011 Mar;185(3):981-6
Common Risks
- Pain at the stimulation site (15.3%)
- New pain (9%)
- Pain at the lead site (5.4%)
- Suspected lead migration (8.4%)
- Infection (6%)
- Transient electric shock (5.5%)
- Changes in bowel function (3%) have all been reported complications of a permanent implantation after a PNE testing
Siegel SW, Catanzaro F, Dijkema HE, et al. Long-term results of a multicenter study on sacral nerve stimulation for treatment of urinary urge incontinence, urgency-frequency, and retention. Urology. 2000;56:87–91
- Medtronic performed a multicenter clinical study including 23 centers worldwide. A total of 581 patients were studied with 219 of them receiving InterStim Therapy. They defined success as increased voided volume with the same or reduced degree of urgency.
- Here are the results:
- Patients had a baseline degree of > 7 voids per day.
- Urge Incontinence (12 month results)
- 45% of patients remained completely dry
- 34% of patients had > 50% reduction in number of wetting episodes
- 70% of patients eliminated heavy leaking episodes
- Urgency-Frequency (12 month results):
- 33% of patients reduced the number of voids by 50%
- 31% of patients reduced the number to normal (4-7 per day)
- 82% of patients improved degree of urgency before a void
Source: Medtronic.com
